Pediatric Speech-Language Therapy

Pediatric Speech-Language Therapy
Center for Pediatric Therapies, Nashua & Parkersburg Clinics
Our therapists are Certified Neurodiversity Affirming Natural Language Acquisition (NLA) trained. Why it matters in the care of your child:
Most commonly, children learn language through something called Analytic Language Development. This means children acquire language by learning that words are single units of meaning and continue to build on this concept to expand language. However, sometimes children develop language from repetition of speech (Gestalt Language Development). This is also a natural way to develop language. It means that early on, children are processing language in chunks or scripts that have a set meaning. These scripts are often tied to emotional experiences and often don't translate literally. Over time, a child will learn to break apart the scripts to recombine the pieces into new combinations, phrases and sentences. In order to help a child who is behind in their communication and language development, it is critical to determine how they are processing what they are hearing. You can be certain our staff is trained to do this!!
What is Speech Therapy?
Our pediatric speech-language pathologists help children learn to successfully communicate their wants, needs, and medical information across a variety of environments. Our speech therapists treat a variety of diagnoses, including developmental delays, oral/facial anomalies, genetic disorders, neurological dysfunction. Additionally, we offer specialized treatment for those with hearing loss and cochlear implants, as well as, treatment for feeding and swallowing disorders. Our therapists work with infants and children to improve:
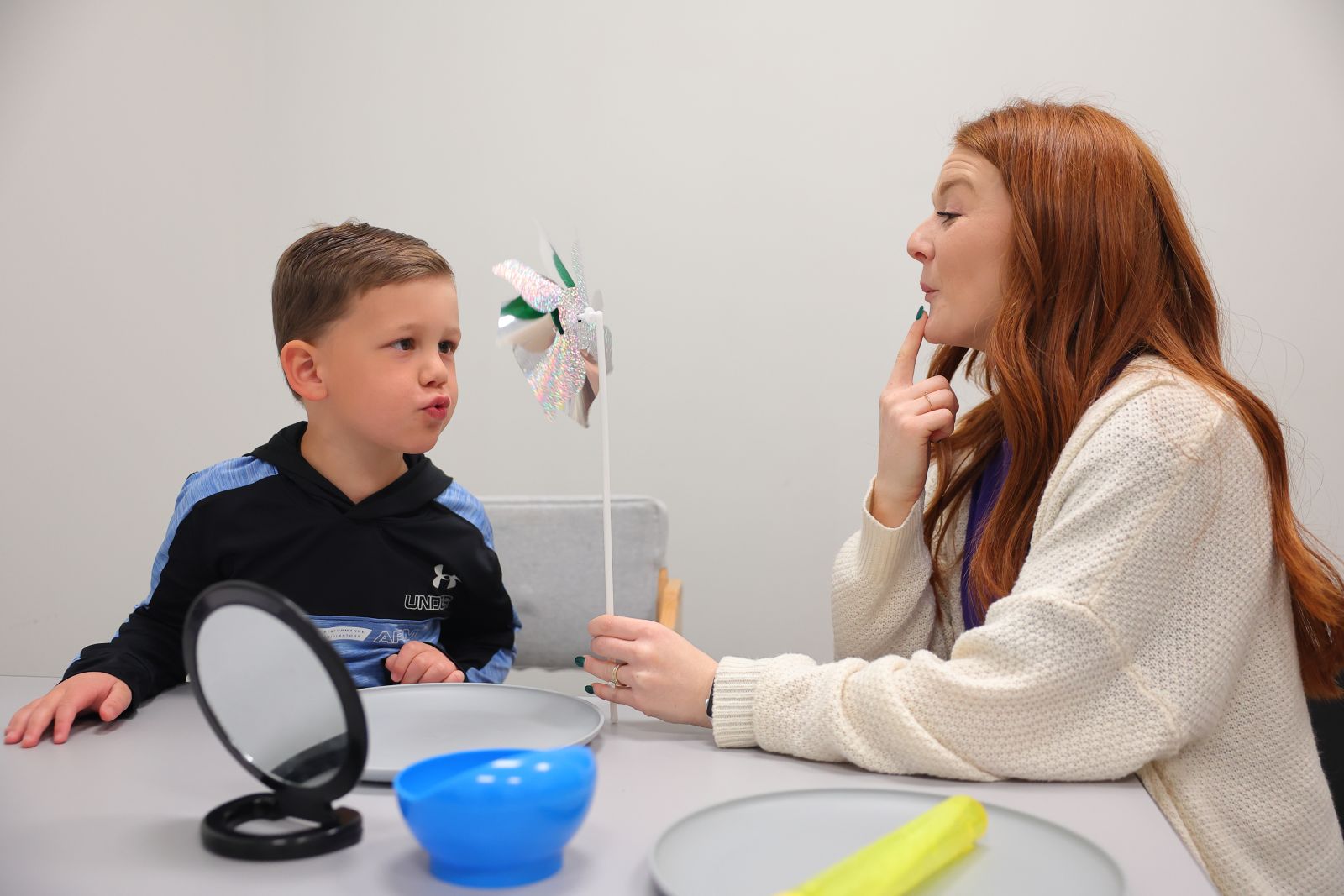
- Verbal speech skills - learning to properly produce sounds in order to be more easily understood by others
- Language comprehension and expression
- Feeding and swallowing problems
- Non-verbal language and social skills
- Attention, memory, abstract reasoning, awareness and executive functions
- Voice and resonance
- Enhancing fluency of speech
- Alternative methods for communication and devices
- Cochlear Implants and Auditory Rehabilitation

How do I know if my child may need Speech Therapy?
Below are some general guidelines that may indicate the need for further assessment by the speech-language pathologist:
Under 18 Months
- No big smile or other warm, joyful expressions by 6 months
- No babbling by 12 months
- Is not using words by 16 months
By 18 Months
- Does not use at least 8-10 meaningful words
- Does not follow simple commands like: "Come here" or "Stop" or "Touch your nose"
.jpg)
By Age 2
- No two-word meaningful phrases (without imitating or repeating)
- Speech is not at least 50% understandable
- Cannot point to pictures of items in books when asked
By Age 3
- Is not using 3 or 4 word sentences
- Speech is not at least 75% or more understandable
- Child is leaving beginning or ends off of most words

By Age 4 to 5
- Is not 100% understandable to strangers despite age appropriate articulation errors (may not be able to say: r, sh, ch, I, or th)
- Is not consistently using 4+ word, complex sentences
- Cannot follow simple 2-step directions
Overall Warning Sings
- ANY loss of speech or babbling or social skills at ANY age
- Never gestures or imitates
- Does not appear to understand speech, or appears to be unable to hear
- Never develops words beyond repeating others over and over
Therapy for Dyslexia
Parkersburg and Waverly Clinic
Offering services to help your child if they are struggling readers and spellers! We use a multisensory approach that uses visual, auditory, and kinesthetic/tactile methods. This is a phonetically based program of reading and spelling which teaches the complete sound structure of language with a great deal of repetition. This treatment may be beneficial for your child if they have a diagnosis of dyslexia, phonological disorders, or other language deficits.

Pediatric Feeding Therapy
Waverly Clinic and Families First Child Care and Learning Center in Waverly
What is a Feeding Disorder?
A child with a feeding disorder may limit what and how much they eat, or they may avoid eating all together and present with difficult behaviors during mealtimes. This avoidance or refusal can lead to weight loss, decreased nutritional status, and compromised physical and cognitive development. A child with a feeding disorder may also present with physical or mechanical difficulties with eating such as: coughing, choking, gagging, or excessive drooling and spilling.

What is Feeding Therapy?
Feeding therapy is a specialized service designed to help patients develop normal and effective feeding patterns and behaviors. Sessions may focus on a variety of mealtime elements including: sensory processing concerns, oral motor skills, negative emotions and/or difficult mealtime behaviors, or any combination of these factors. Some of the most common feeding therapy goals include:
- Decrease texture aversions and/or avoidances
- Increase variety of foods eaten
- Increase total volume of food/liquid consumed in one sitting
- Improve mealtime behaviors and emotions or attitudes associated with eating and swallowing
- Improve efficiency of drinking and swallowing, including assistance with learning to self-feed
- Exercise and stretch oral/facial structures to improve strength, range of motion, and coordination for more effective oral motor skills.

How do I know if my child may need feeding therapy?
Below are some general guidelines that may indicate the need for further assessment by a feeding therapist.
- Difficulty chewing foods, may swallow food in whole pieces.
- Difficulty swallowing foods or refusing to swallow certain food consistencies.
- Gags on, avoids, or is very sensitive to certain food textures, temperatures, and/or flavors.
- Struggles to control and coordinate food in the mouth while chewing or swallowing.
- Frequently coughs, gags, or chokes when eating.
- Frequently vomits during or immediately after eating/drinking.
- Refuses or rarely tries new foods.
- Negative mealtime behaviors (infant cries, arches, pulls away from food; child refuses to eat, tantrums at mealtimes or "shuts-down" and does not engage in mealtime).
- Infant demonstrating signs of difficulty with coordinating the suck/swallow/breath pattern during bottle or breastfeeding.
- Feeding time takes longer than 30 minutes for infants, and 30 to 40 minutes for toddlers or young children.
- Known to be "picky eater" who eats a limited variety of foods or consistencies (less than 20 foods)
- G-Tube or NG-Tube dependency (with or without gastro-esophageal reflux disease, GERD)
- Poor weight gain or failure to thrive
- Cranio-facial anomalies such as cleft-lip and palate

I think my child may need to be seen by a speech therapist. What should I do next?
Always consult with your primary care physician with any concerns regarding your child's development, including feeding and swallowing concerns. A doctor's referral is required to initiate speech therapy services as well as a feeding evaluation and associated therapies. Speech therapy, including feeding therapy, is covered by most private insurances and Medicaid. Please call your insurance company for details about your specific coverage. For appointment information or questions regarding your child's individual skills and development, please contact any of the Taylor Physical Therapy clinics.

